Modern medicine would likely seem like magic to those who lived in the early 20th century. While medicine in the early parts of the 20th century was far advanced from the medieval days of leeches, most of their treatments were still misguided and often even barbaric by our modern standards. Many of the devices used in this treatments look more like something from a serial killer’s basement than state of the art medical technology. From nightmarish steampunk styled prosthetic limbs to treatment with deadly radium, many of the procedures of the early 20th century would have seemed more like torture than healing.
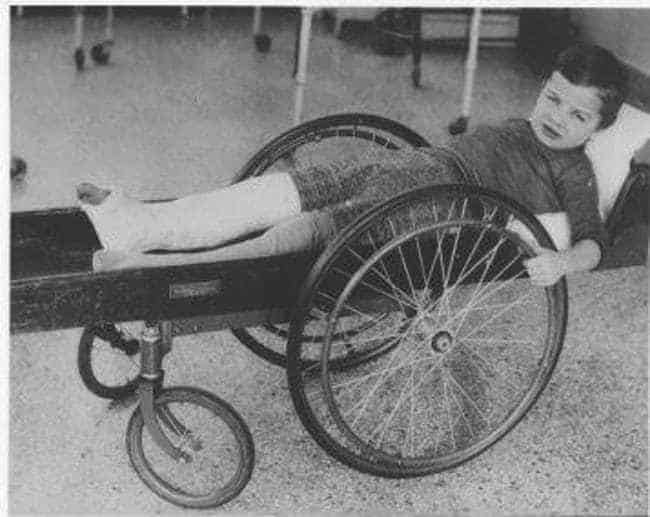
18. Early Wheelchairs
Wheelchairs have likely existed, in some rudimentary form, since between the 6th and 4th centuries B.C alongside the invention of wheeled furniture. However, they didn’t enter Europe until the 12th century A.D., and these early models were extraordinarily primitive and more akin to wheelbarrows than the modern chairs we have today. The earliest recognizable, self-propelled wheelchair didn’t exist until the 17th century, when German inventors Johann Hautsch and Stephan Farfler independently made several prototypes. Farfler himself was disabled and created what was called an “invalid chair” that consisted of three wheels controlled by various cranks and levers.
Until the 19th century, wheelchairs were primarily used by the wealthy as a means of transport for disabled people. The 19th century saw the rise of cheaper devices made for use in hospital settings to transport disabled patients. These models were more accessible for middle-class disabled people as well. The many disabled veterans left after the US Civil War led to a rise in the production of wooden wheelchairs, which were basically hard wooden seats on wheels. More modern bicycle-like wheels were introduced at the end of the 19th century, but these wheelchairs were still cumbersome and only fit for indoor use.
The collapsible metal tube wheelchair that we use today was not invented until the 20th century. This innovation allowed disabled people far more mobility regarding travel and outdoor use. Electric wheelchairs, rather than self-propelled models, were developed after World War II.

